The term “sciatica” is thought to have been first coined by Hippocrates, the father of medicine, sometime around 400 BC. The word evolved from the Greek words "ischias" (hip pain) and "ischiadikos" (of the hip). It describes the presence of pain, numbness, and/or tingling coursing from the low back or hip extending into the thigh, calf, and even foot along the path of the sciatic nerve – the largest nerve in the body. Weakness in the lower limb may also develop. Technically sciatica is not a primary problem, but rather a symptom stemming from other causes irritating the nerve. Proposed sources include a bulging or herniated lumbar intervertebral disc, bone spurs and stenosis, overactive muscles like the piriformis, and in rarer cases tumors and trauma. Yet these conditions are frequently not present in many cases of sciatica, meaning that the presence of these issues does not always trigger sciatica. Diagnosis is frequently rendered based simply on symptom report. A straight leg raise test (also called Lasegue test) may be positive due to tension applied to an irritated sciatic nerve. Imaging such as X-ray and MRI may be employed to aid diagnosis, but can also be misleading and not correlate with symptom presentation.
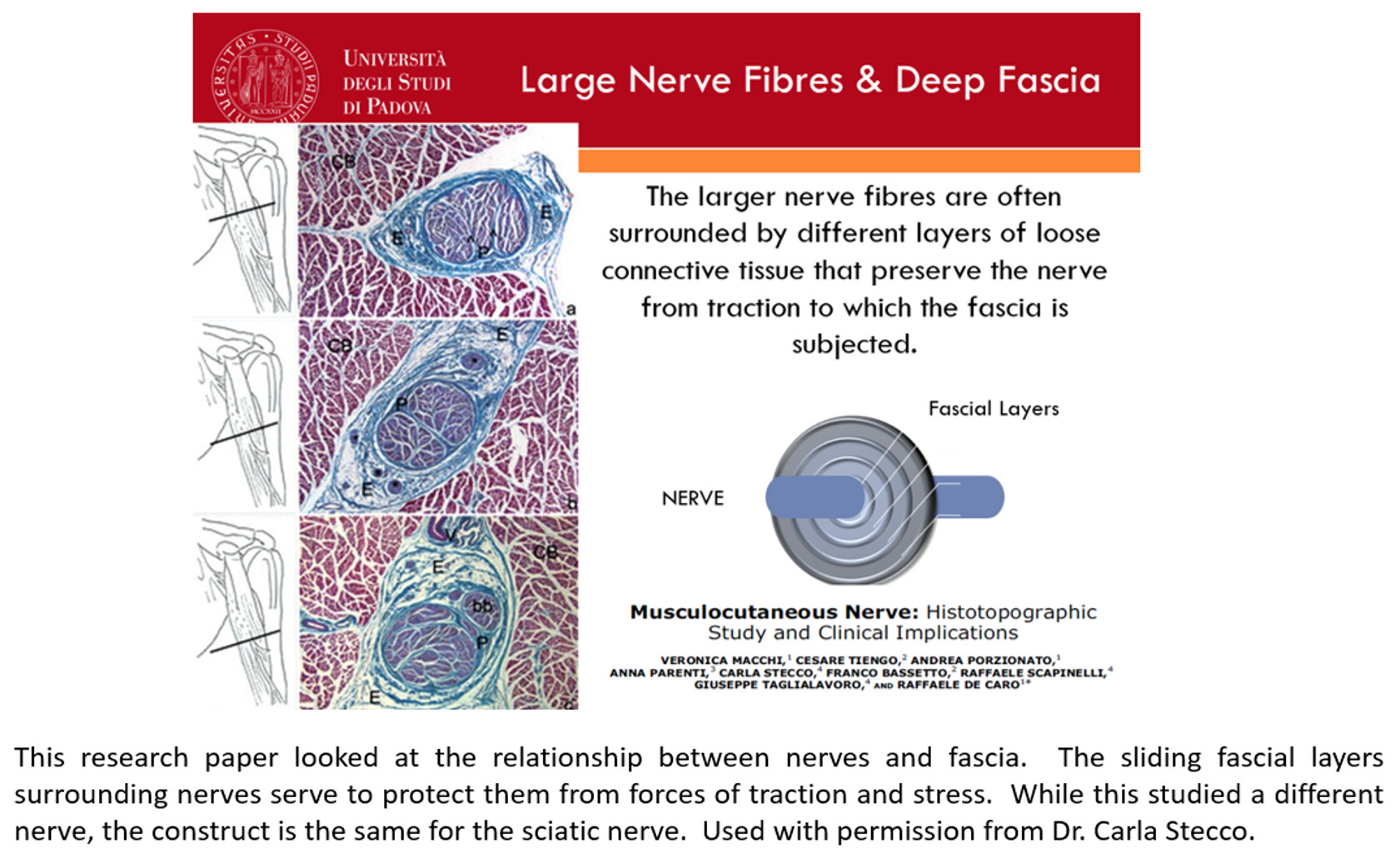
It's good to appreciate that there is typically a provoking element behind these proposed sources of sciatica, making them not the actual origin of the problem. For instance, in the case of the piriformis, the muscle cannot decide on its own to compress the sciatic nerve unless the nervous system facilitates it. The real question is what is facilitating the nervous system to do this? In the case of such mysteries as sciatica, it's always good to consider the anatomy and physiology including the fascia. The ubiquitous nature of fascia positions it to surround the sciatic nerve along its entire course – from low back to foot. The fascia serves as a protective element for the nerves, and accommodates traction forces present in everyday movements. But this construct is counting on the integrity of the sliding system between the tissue layers. Compromise this slide at one or more points along the neural pathway and sciatic symptoms may manifest.
Traditional management strategies include rest, mobilization / manipulation, exercise, medications, injections, and surgery. While potentially helpful in some respects, none of these interventions takes into account the role of the fascia surrounding and influencing the sciatic nerve. Identification and abolishment of fascial densifications along the neural pathway can restore lost slide in the layers and remove tension and pull on the nerve. Appreciating the role an old injury into the lower limb may play is crucial for resolving the problem. – like an old ankle sprain or foot fracture.
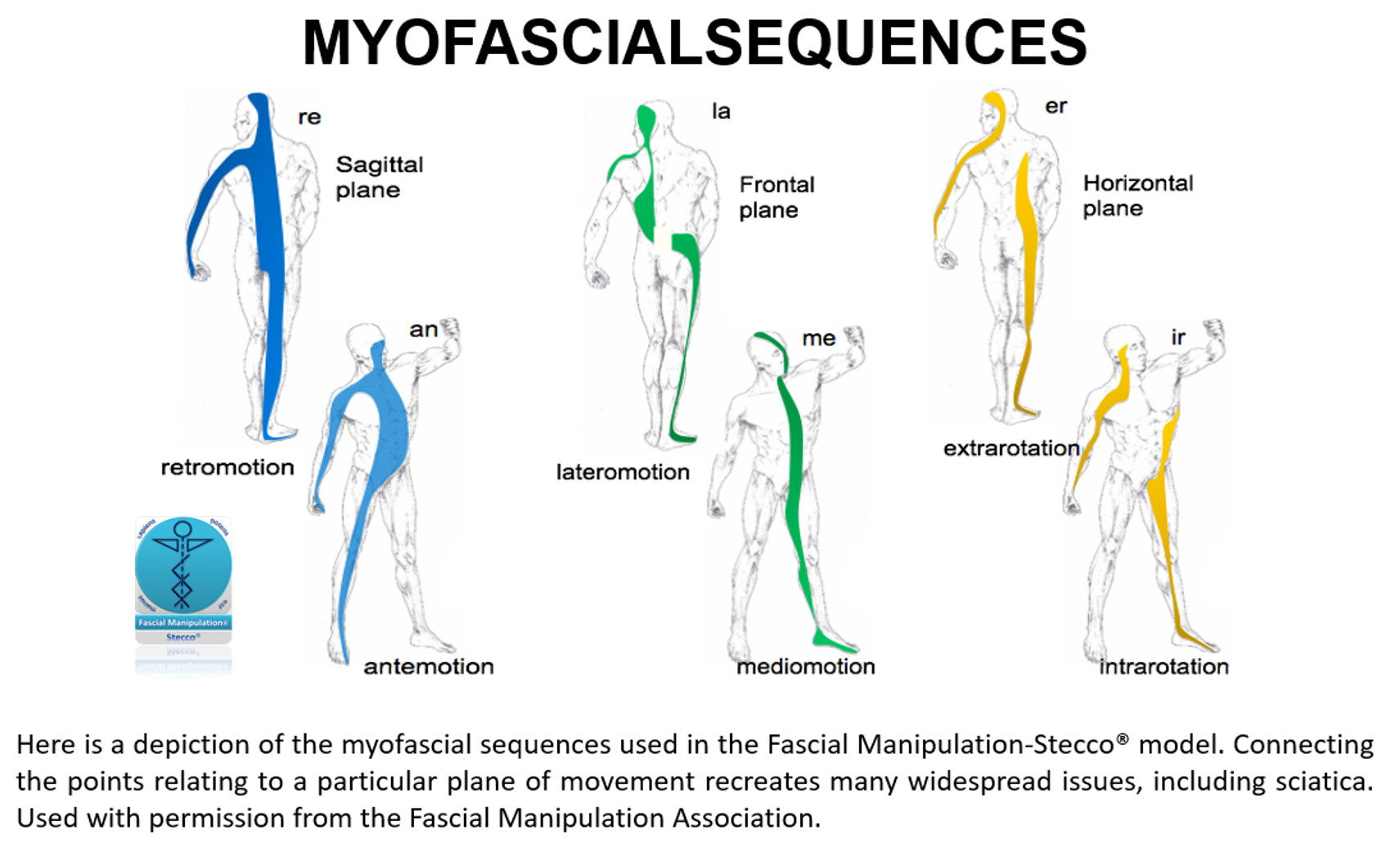
Don't let sciatica slow you down when there is much that can be done to resolve it. To learn more about how fascial work please explore my website and feel free to give me a call, send a text, book an exploratory session, or schedule a consult. You have options – act on them!





